Bayesian Learning Based Optimization of Meal Bolus Dosage for Intelligent Glucose Management
-
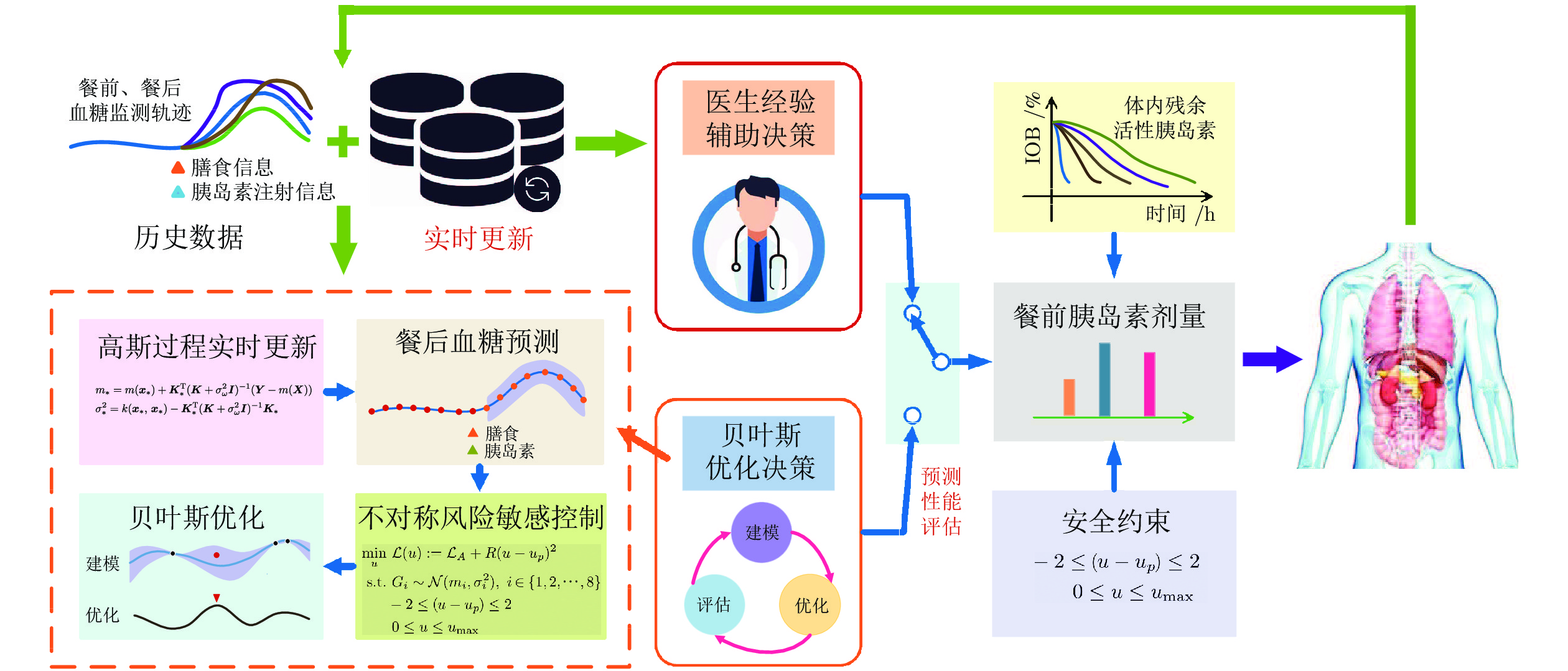
摘要: 餐前胰岛素剂量精准决策是改善糖尿病患者血糖管理的关键. 临床治疗中胰岛素剂量调整一般在较短时间内完成, 具有典型的小样本特征; 数据驱动建模在该情形下无法准确学习患者餐后血糖代谢规律, 难以确保胰岛素剂量的安全和有效决策. 针对这一问题, 设计一种临床经验辅助的餐前胰岛素剂量自适应优化决策框架, 构建高斯过程血糖预测模型和模型有效性在线评估机制, 提出基于历史剂量和临床经验决策约束的贝叶斯优化方法, 实现小样本下餐后血糖轨迹的安全预测和餐前胰岛素注射剂量的优化决策. 该方法的安全性和有效性通过美国食品药品监督管理局接受的UVA/Padova T1DM平台测试结果和1型糖尿病患者实际临床数据决策结果充分验证. 可为餐前胰岛素剂量智能决策及临床试验提供方法基础和技术支持, 也为中国糖尿病患者血糖管理水平的有效改善, 提供了精准医学治疗手段.Abstract: Precise decision of preprandial insulin bolus is of crucial importance to achieving enhanced glucose management for patients with diabetes. Insulin dosage adjustment in current clinical practice normally needs to be completed in a relatively short period of time and thus the data size is typically small. It would be consequently challenging to accurately learn the postprandial glucose metabolism through data-driven modelling techniques and to further ensure the safe and efficient insulin dosage decision. For this problem, a clinical-experience-assisted adaptive preprandial insulin bolus decision framework is proposed in this work. To achieve safe prediction of the postprandial glucose traces and optimal decision of the preprandial insulin dosage with limited training data, a Gaussian process based glucose prediction model and an online model efficiency assessment mechanism are constructed, and a Bayesian optimization method with historical data exploitation and clinical-experience guided decision constraints is proposed. The safety and effectiveness of the proposed method are extensively validated through in silico results of the US Food and Drug Administration accepted UVA/Padova T1DM simulator and advisory mode analysis based on clinical data from a subject with type 1 diabetes. The obtained results provide methodological and technical support for intelligent meal bolus decision and the forthcoming clinical studies, and introduce a precision medicine solution to effectively improved glucose management for Chinese patients with diabetes mellitus.
-
表 1 方法参数
Table 1 The parameters of the proposed method
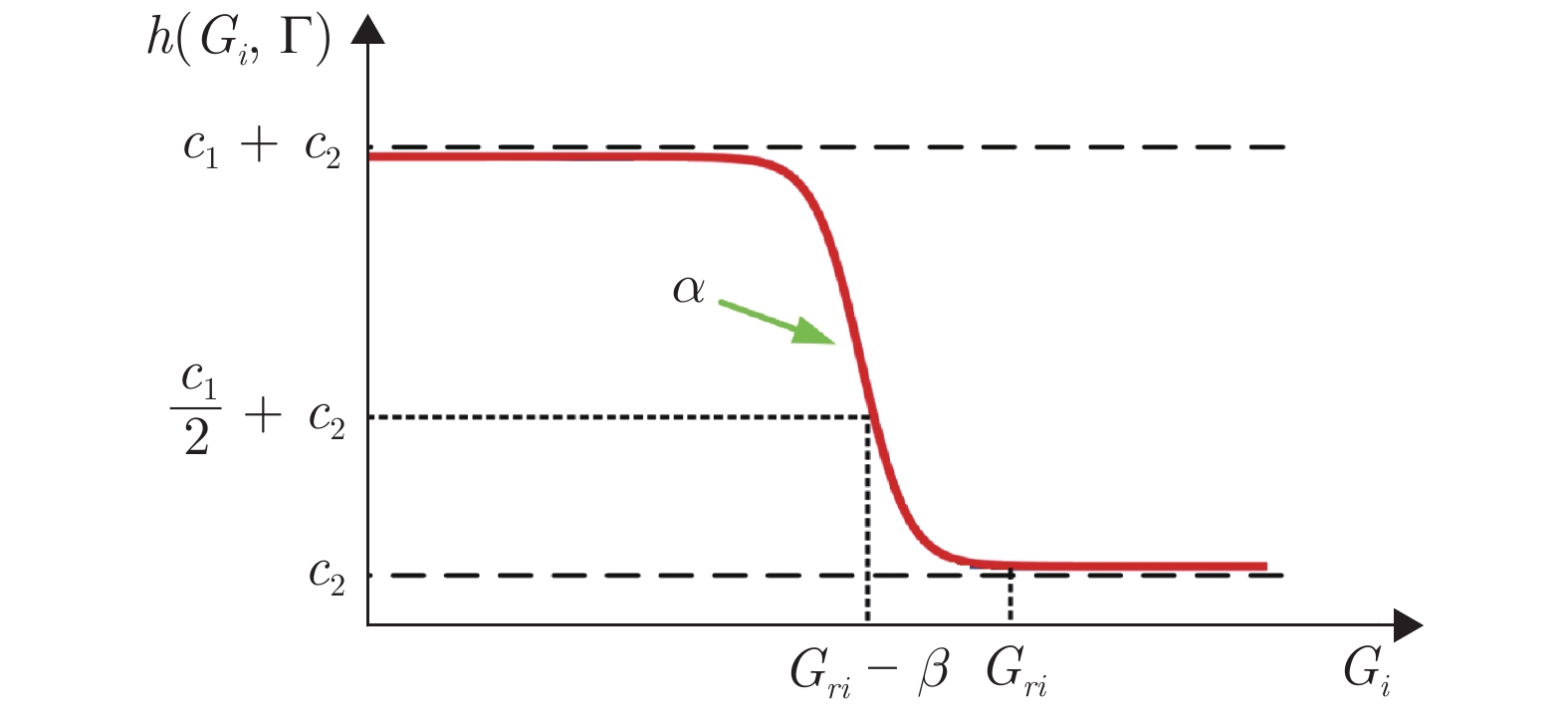
变量 含义 值 $ \gamma $ 风险敏感参数 −2 $ R $ 权重系数 10 $ u_{\max} $ 最大剂量约束值 20 $ M $ 最大优化次数 25 $ {Q\mathit{\boldsymbol{}}}_b $ 基准惩罚矩阵 $\rm{diag}\{0.0025,\cdots, 0.0025,$ $0.005,0.005\}$ $ \Gamma $ 不对称惩罚强度 $ \{1,10,5,1\} $ $ {G\mathit{\boldsymbol{}}}_r $ 餐后血糖控制目标 $[110,130,150,170, 160,$ $150,150,150]^{\rm{T} }$ $ \Delta u $ 评估增量 $ 2 $ $ G_h $ 餐后血糖高阈值 $ 120 $ $ G_l $ 餐后血糖低阈值 $ 80 $ $ \Delta G $ 餐前血糖均值增量 $ 30 $ 表 2 前期餐前剂量正常情形下$r = 1 $血糖控制评估结果 (%)
Table 2 Evaluation results of the glucose control in the case of normal boluses in the early stage when$r=1 $ (%)
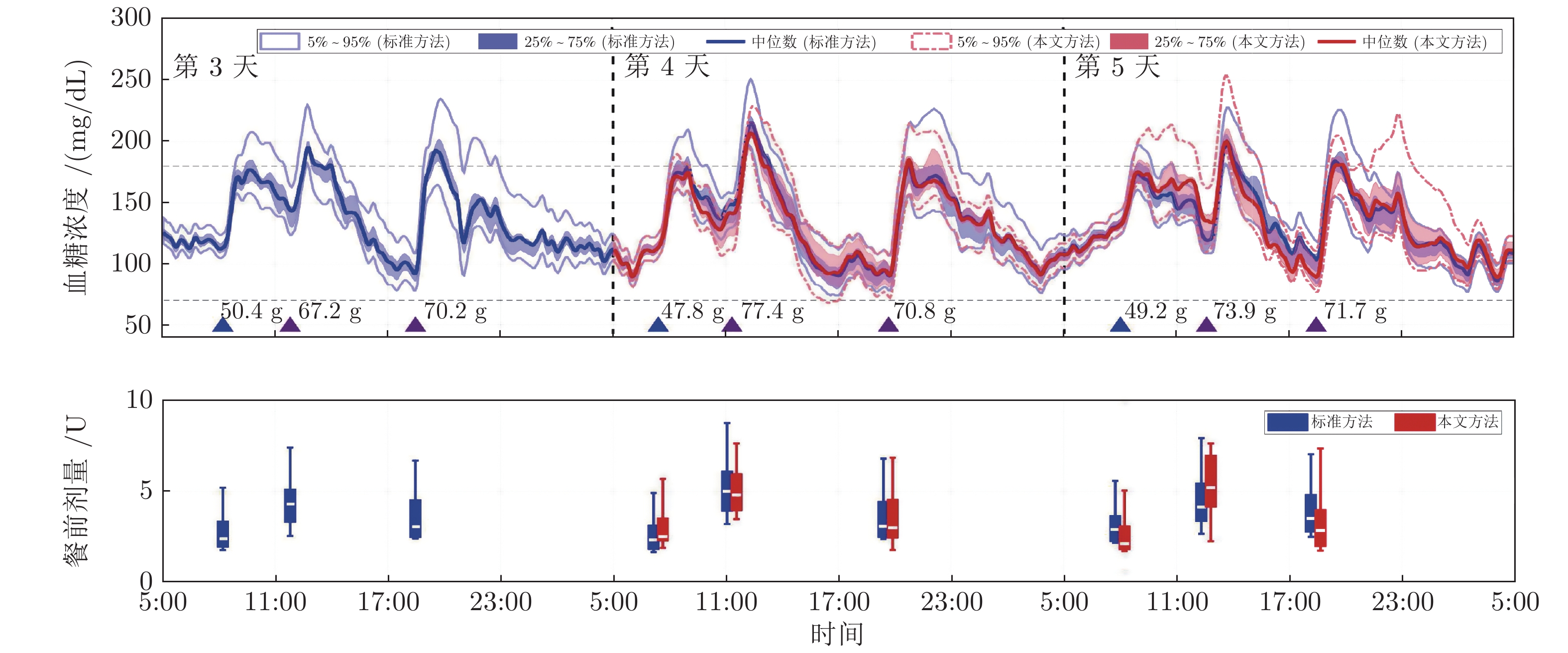
评价指标 标准方法 本文方法 $ p $ 值 < 54 mg/dL (%) 0 (0) 0 (0) 1.000 < 70 mg/dL (%) 0 (0) 0 (0) 1.000 70 ~ 180 mg/dL (%) 93.6 (7.5) 92.3 (6.6) 0.188 > 250 mg/dL (%) 0 (0) 0 (0) 1.000 血糖平均值(mg/dL) 133.2 (9.4) 132.5 (14.0) 1.000 标准差(mg/dL) 30.2 (7.0) 30.3 (4.4) 0.037 7:00血糖平均值(mg/dL) 109.8 (11.0) 109.3 (8.0) 0.195 表 3 前期餐前剂量偏少/偏多情形下血糖控制评估结果(%)
Table 3 Evaluation results of the glucose control in the case of under-estimated/over-estimated boluses in the early stage (%)
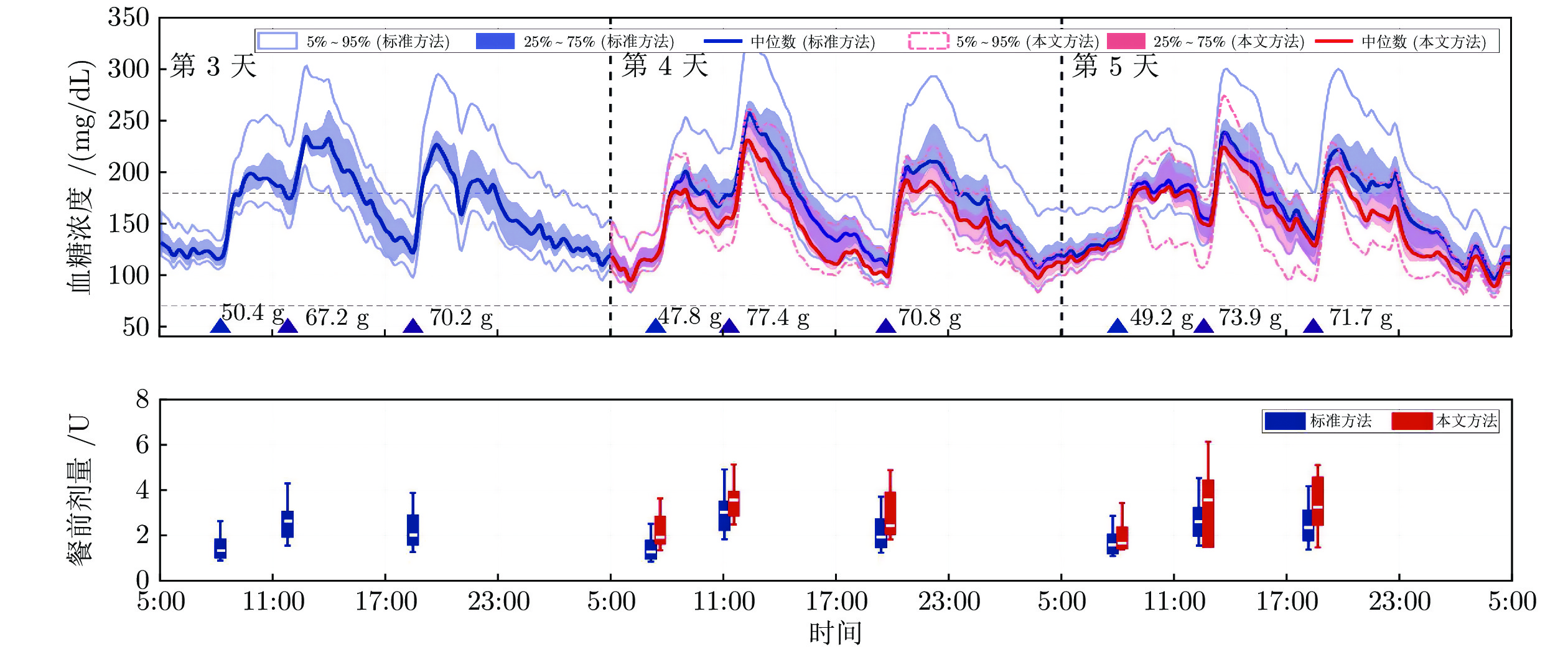
评价指标 前期餐前剂量偏少($ r = 0.5 $) 前期餐前剂量偏多($ r = 1.5 $) 标准方法 本文方法 $ p $ 值 标准方法 本文方法 $ p $ 值 < 54 mg/dL (%) 0 (0) 0 (0) 1.000 1.6 (3.8) 0 (0) 0.031 < 70 mg/dL (%) 0 (0) 0 (0) 1.000 6.5 (7.8) 0 (1.4) 0.008 70 ~ 180 mg/dL (%) 64.8 (23.6) 77.1 (18.4) 0.004 91.6 (6.9) 95.6 (2.6) 0.232 > 250 mg/dL (%) 1.0 (4.5) 0 (0) 0.031 0 (0) 0 (0) 1.000 血糖平均值 (mg/dL) 162.1 (29.2) 148.7 (16.8) 0.004 114.9 (9.0) 125.6 (10.5) 0.002 标准差 (mg/dL) 37.9 (7.6) 35.8 (5.6) 0.010 29.4 (6.2) 30.9 (5.3) 0.049 7:00血糖平均值 (mg/dL) 118.0 (20.0) 113.0 (9.5) 0.008 104.8 (10.0) 108.0 (12.5) 0.039 表 4 膳食扰动下血糖控制评估结果(%)
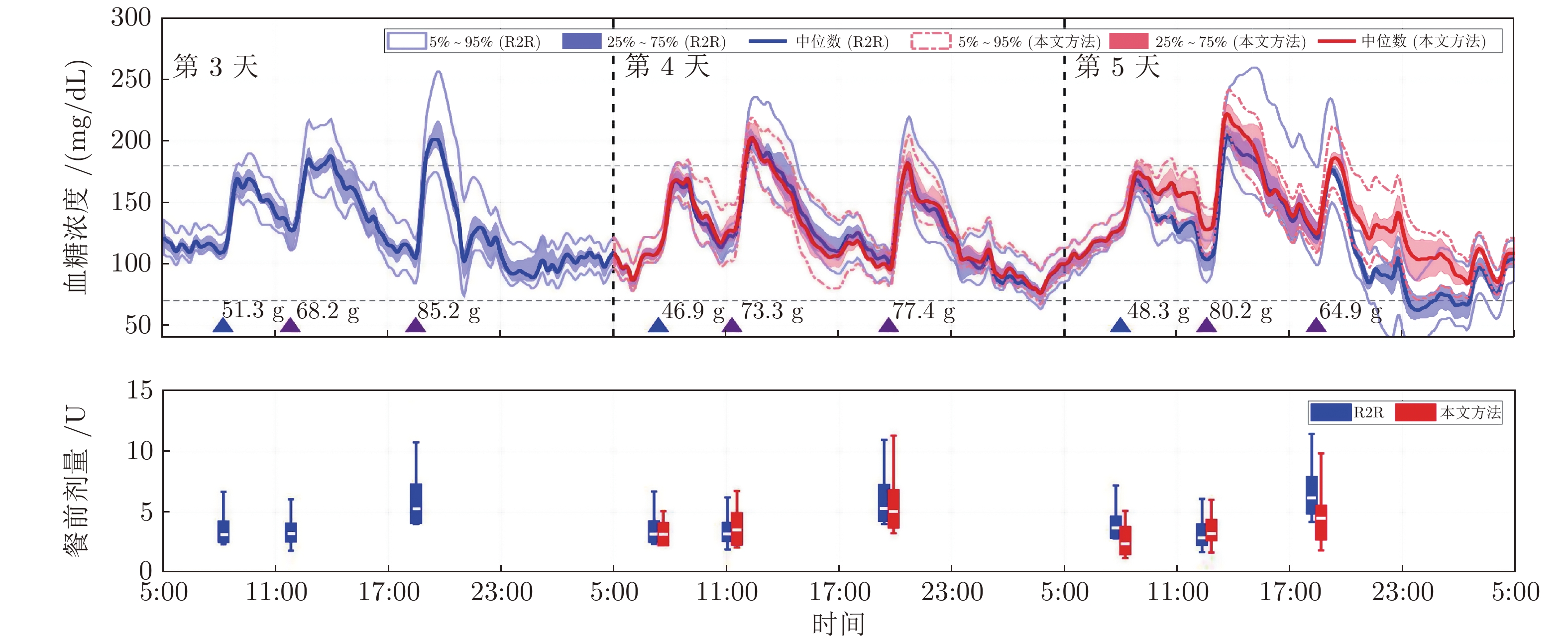
Table 4 Evaluation results of the glucose control in the case of meal disturbance (%)
评价指标 R2R 本文方法 $ p $ 值 $< $54 mg/dL (%) 0 (0.7) 0 (0) 0.250 $< $70 mg/dL (%) 3.6 (8.3) 0 (0) 0.016 70 ~ 180 mg/dL (%) 87.7 (13.0) 89.1 (5.6) 0.625 $>$250 mg/dL (%) 0 (0) 0 (0) 1.000 血糖平均值(mg/dL) 123.8 (10.6) 131.3 (7.0) 0.006 标准差(mg/dL) 36.0 (9.4) 34.9 (7.5) 0.432 7:00血糖平均值(mg/dL) 102.8 (12.0) 103.8 (8.5) 0.004 -
[1] 纪立农. 活的更长、活得更好——糖尿病与“健康中国2030”. 中国糖尿病杂志, 2019, 27(01):1-2 doi: 10.3969/j.issn.1006-6187.2019.01.001Ji Li-Nong. Live longer and live better---diabetes and "Healthy China 2030". Chinese Journal of Diabetes, 2019, 27(01):1-2 doi: 10.3969/j.issn.1006-6187.2019.01.001 [2] 纪立农. 胰岛素无针注射器的中国研究:FREE研究. 中华糖尿病杂志, 2020, 12(9):674-676 doi: 10.3760/cma.j.cn115791-20200811-00497Ji Li-Nong. A Chinese study on needle-free injection in type 2 diabetes mellitus: FREE Study. Chinese Journal of Diabetes, 2020, 12(9):674-676 doi: 10.3760/cma.j.cn115791-20200811-00497 [3] Liu W, McGuire H C, Kissimova-Skarbek K, Zhou X, Han X, Wang Y, et al. Factors associated with resistance to complications in long-standing type 1 diabetes in China. Endocrine Research, 2020, 45(1):1-8 doi: 10.1080/07435800.2019.1624567 [4] Schiffrin A, Belmonte M M. Multiple daily self-glucose monitoring: its essential role in long-term glucose control in insulin-dependent diabetic patients treated with pump and multiple subcutaneous injections. Diabetes Care, 1982, 5(5):479-484 doi: 10.2337/diacare.5.5.479 [5] Quiroz G. The evolution of control algorithms in artificial pancreas: A historical perspective. Annual Reviews in Control, 2019, 48:222-232 doi: 10.1016/j.arcontrol.2019.07.004 [6] Kovatchev B. A century of diabetes technology: signals, models, and artificial pancreas control. Trends in Endocrinology and Metabolism, 2019, 30(7):432-444 doi: 10.1016/j.tem.2019.04.008 [7] 史大威, 杨肖, 蔡德恒, 牟治宇, 刘蔚, 纪立农. 基于胰岛素基础率估计的人工胰腺系统自抗扰控制. 自动化学报, 2021, 47(5):1043-1057Shi Da-Wei, Yang Xiao, Cai De-Heng, Mou Zhi-Yu, Liu Wei, Ji Li-Nong. Active disturbance rejection control for artificial pancreas system based on insulin basal rate estimation. Acta Automatica Sinica, 2021, 47(5):1043-1057 [8] El Fathi A, Raef Smaoui M, Gingras V, Boulet B, Haidar A. The artificial pancreas and meal control: An overview of postprandial glucose regulation in type 1 diabetes. IEEE Control Systems, 2018, 38(1):67-85 doi: 10.1109/MCS.2017.2766323 [9] Klonoff D. The current status of bolus calculator decision-support software. Journal of Diabetes Science and Technology, 2012, 6(5):990-994 doi: 10.1177/193229681200600501 [10] Shashaj B, Busetto E, Sulli N. Benefits of a bolus calculator in pre- and postprandial glycaemic control and meal flexibility of paediatric patients using continuous subcutaneous insulin infusion (CSII). Diabetic Medicine, 2008, 25(9):1036-1042 doi: 10.1111/j.1464-5491.2008.02549.x [11] Herrero P, Pesl P, Bondia J, Reddy M, Oliver N, Georgiou P, et al. Method for automatic adjustment of an insulin bolus calculator: In silico robustness evaluation under intra-day variability. Computer Methods and Programs in Biomedicine, 2015, 119(1):1-8 doi: 10.1016/j.cmpb.2015.02.003 [12] Schiavon M, Dalla Man C, Cobelli C. Insulin sensitivity indexbased optimization of insulin to carbohydrate ratio in silico study shows efficacious protection against hypoglycemic events caused by suboptimal therapy. Diabetes Technology and Therapeutics, 2018, 20(2):98-105 doi: 10.1089/dia.2017.0248 [13] Torrent-Fontbona F, Lopez B. Personalized adaptive CBR bolus recommender system for type 1 diabetes. IEEE Journal of Biomedical and Health Informatics, 2019, 23(1):387-394 doi: 10.1109/JBHI.2018.2813424 [14] Turksoy K, Hajizadeh I, Samadi S, Feng J, Sevil M, Park M, et al. Real-time insulin bolusing for unannounced meals with artificial pancreas. Control Engineering Practice, 2017, 59:159-164 doi: 10.1016/j.conengprac.2016.08.001 [15] Herrero P, Bondia J, Adewuyi O, Pesl P, El-Sharkawy M, Reddy M, et al. Enhancing automatic closedloop glucose control in type 1 diabetes with an adaptive meal bolus calculator - in silico evaluation under intra-day variability. Computer Methods and Programs in Biomedicine, 2017, 146:125-131 doi: 10.1016/j.cmpb.2017.05.010 [16] Shi D, Dassau E, Doyle III F J. Multivariate learning framework for long-term adaptation in the artificial pancreas. Bioengineering and Translational Medicine, 2019, 4(1):61-74 doi: 10.1002/btm2.10119 [17] 侯忠生, 许建新. 数据驱动控制理论及方法的回顾和展望. 自动化学报, 2009, 35(6):650-667 doi: 10.3724/SP.J.1004.2009.00650Hou Zhong-Sheng, Xu Jian-Xin. On data-driven control theory: the state of the art and perspective. Acta Automatica Sinica, 2009, 35(6):650-667 doi: 10.3724/SP.J.1004.2009.00650 [18] 代伟, 柴天佑. 数据驱动的复杂磨矿过程运行优化控制方法. 自动化学报, 2014, 40(9):2005-2014Dai Wei, Chai Tian-You. Data-driven optimal operational ccontrol of complex grinding processes. Acta Automatica Sinica, 2014, 40(9):2005-2014 [19] 郜传厚, 渐令, 陈积明, 孙优贤. 复杂高炉炼铁过程的数据驱动建模及预测算法. 自动化学报, 2009, 35(6):725-730 doi: 10.3724/SP.J.1004.2009.00725Gao Chuan-Hou, Jian Ling, Chen Ji-Ming, Sun You-Xian. Data-driven modeling and predictive algorithm for complex blast furnace ironmaking process. Acta Automatica Sinica, 2009, 35(6):725-730 doi: 10.3724/SP.J.1004.2009.00725 [20] Wang Y, Dassau E, Doyle III F J. Closed-loop control of artificial pancreatic beta-cell in type 1 diabetes mellitus using model predictive iterative learning control. IEEE Transactions on Biomedical Engineering, 2010, 57(2):211-219 doi: 10.1109/TBME.2009.2024409 [21] Wang Y, Zhang J, Zeng F, Wang N, Chen X, Zhang B, et al. "Learning" can improve the blood glucose control performance for type 1 diabetes mellitus. Diabetes Technology and Therapeutics, 2017, 19(1):41-48 doi: 10.1089/dia.2016.0328 [22] Song L, Liu C, Yang W, Zhang J, Kong X, Zhang B, et al. Glucose outcomes of a learning-type artificial pancreas with an unannounced meal in type 1 diabetes. Computer Methods and Programs in Biomedicine, 2020, 191(105416):1-9 [23] Cai D, Liu W, Ji L, Shi D. Bayesian optimization assisted meal bolus decision based on Gaussian processes learning and risk-sensitive control. Control Engineering Practice, 2021, 114(104881):1-11 [24] 中华医学会糖尿病学分会. 中国1型糖尿病胰岛素治疗指南. 中华糖尿病杂志, 2016, 8(10):591-597 doi: 10.3760/cma.j.issn.1674-5809.2016.10.005Chinese Diabetes Society. Insulin therapy guidelines for type 1 diabetes in China. Chinese Journal of Diabetes, 2016, 8(10):591-597 doi: 10.3760/cma.j.issn.1674-5809.2016.10.005 [25] Dalla Man C, Micheletto F, Lv D, Breton M, Kovatchev B, Cobelli C. The UVA/PADOVA type 1 diabetes simulator: New features. Journal of Diabetes Science and Technology, 2014, 8(1):26-34 doi: 10.1177/1932296813514502 [26] Gillis R, Palerm C C, Zisser H, Jovanovic L, Seborg D E, Doyle III F J. Glucose estimation and prediction through meal responses using ambulatory subject data for advisory mode model predictive control. Journal of Diabetes Science and Technology, 2007, 1(6):825-833 doi: 10.1177/193229680700100605 [27] Rasmussen C E, Williams C K I. Gaussian Processes for Machine Learning. Cambridge: The MIT Press, 2006. [28] Hovorka R, Canonico V, Chassin L J, Haueter U, Massi-Benedetti M, Federici M O, et al. Nonlinear model predictive control of glucose concentration in subjects with type 1 diabetes. Physiological Measurement, 2004, 25(4):905-920 doi: 10.1088/0967-3334/25/4/010 [29] Deisenroth M P, Fox D, Rasmussen C E. Gaussian processes for data-efficient learning in robotics and control. IEEE Transactions on Pattern Analysis and Machine Intelligence, 2015, 37(2):408-423 doi: 10.1109/TPAMI.2013.218 [30] Jain A, Nghiem T X, Morari M, Mangharam R. Learning and control using Gaussian processes. In: Proceedings of the 9th ACM/IEEE International Conference on Cyber-physical Systems. Porto, Portugal: 2018. 140−149 [31] Gondhalekar R, Dassau E, Doyle III F J. Periodic zone-MPC with asymmetric costs for outpatient-ready safety of an artificial pancreas to treat type 1 diabetes. Automatica, 2016, 71:237-246 doi: 10.1016/j.automatica.2016.04.015 [32] Lee J B, Dassau E, Gondhalekar R, Seborg D E, Pinsker J E, Doyle III F J. Enhanced model predictive control (eMPC) strategy for automated glucose control. Industrial and Engineering Chemistry Research, 2016, 55(46):11857-11868 doi: 10.1021/acs.iecr.6b02718 [33] Whittle P, Kuhn J. A hamiltonian formulation of risk-sensitive linear/quadratic/Gaussian control. International Journal of Control, 1986, 43(1):1-12 doi: 10.1080/00207178608933445 [34] Yang X, Maciejowski J. Risk-sensitive model predictive control with Gaussian process models. IFAC-PapersOnLine, 2015, 48(28):374-379 doi: 10.1016/j.ifacol.2015.12.156 [35] Pan Y, Boutselis G, Theodorou E. Efficient reinforcement learning via probabilistic trajectory optimization. IEEE Transactions on Neural Networks and Learning Systems, 2018, 29(11):5459-5474 doi: 10.1109/TNNLS.2017.2764499 [36] Shahriari B, Swersky K, Wang Z, Adams R P, De Freitas N. Taking the human out of the loop: A review of bayesian optimization. Proceedings of the IEEE, 2015, 104(1):148-175 [37] Jones D R, Schonlau M, Welch W J. Efficient global optimization of expensive black-box functions. Journal of Global Optimization, 1998, 13(4):455-492 doi: 10.1023/A:1008306431147 [38] Toffanin C, Visentin R, Messori M, Palma F D, Magni L, Cobelli C. Towards a run-to-run adaptive artificial pancreas: In silico results. IEEE Transactions on Biomedical Engineering, 2018, 65(4):479-488 [39] Liu W, Chen J, He L, Cai X, Zhang R, Gong S, et al. Flash glucose monitoring data analyzed by detrended fluctuation function on β cell function and diabetes classification. Diabetes Obesity and Metabolism, 2021, 23(3):774-781 doi: 10.1111/dom.14282 -




 下载:
下载: